
Should a veterinarian treat a patient as if the pet were her own?
Last year I was asked to do just this by clients I had just met. But making decisions as if a pet is your own is hard thing to do. What I may choose for my pet may not be right for someone else.
Case in point: Paige.
 I adopted my once-in-a-lifetime dog, a 13-month-old black Labrador, during my first month of veterinary school at Cornell. She was with me through veterinary school and graduation, an internship in New York City, oncology positions at Duke and back at Cornell, my residency back in NYC, a wedding, a move out to California, then back to New York, and the birth of my 2 sons. She was by my side for it all, and she was perfect. I used to say I would give her my kidney if she needed it.
I adopted my once-in-a-lifetime dog, a 13-month-old black Labrador, during my first month of veterinary school at Cornell. She was with me through veterinary school and graduation, an internship in New York City, oncology positions at Duke and back at Cornell, my residency back in NYC, a wedding, a move out to California, then back to New York, and the birth of my 2 sons. She was by my side for it all, and she was perfect. I used to say I would give her my kidney if she needed it.
I was pretty attached to Paige, to say the least. She died 8 years ago, and she never needed my kidney, but I would have given it to her if I could have.
About the same time, Chandler, an adorable 8-year-old Papillon, was referred to me for treatment. His tumor involved the in the prostate and urethra. The urethra is the tube that connects urine from the bladder to the outside world. Sometimes dogs like Chandler have a hard time urinating from the urethral involvement, but Chandler was having a hard time defecting from the prostate tumor pressing on his colon. His owners had come to me to consider a procedure called CyberKnife, a precise radiation of the tumor.
As I was telling the clients about the cancer, the treatment options and the prognosis, I could see the bond they both had with Chandler. They looked me right in the eye, and asked me to treat him like he was my own pet.
I don’t normally agree to this. I prefer to educate, to guide, to help, and then to let the owners make the best decision for themselves and their pets. But Chandler’s owners and I had connected at that moment. So I promised them what they asked of me: I would treat Chandler as if he were my own dog, Paige.
[tweetthis]I promised them what they asked of me: I would treat Chandler like my own dog.[/tweetthis]
Complications for Plan A
In order to be a candidate for CyberKnife, the pet’s prostate tumor cannot extend in to bladder. That’s because hollow organs like the bladder can rupture after radiation treatments, as the invasive tumor is killed from radiation and there is no normal tissue in that area. At the original appointment, I had determined the cancer had spread to the local lymph nodes under his lumbar spine, but not beyond, and his chest was clear. Ideally we would also radiate the lymph nodes, in addition to the tumor itself, which added a significant cost to the already expensive CyberKnife treatment.
“Would you do it, Dr. Sue?” they asked. And I told them honestly that I would, were I in their situation. But then I asked them to make sure that was the right choice – or at least, the best choice – for them and for Chandler.
They decided to go ahead.
But as the radiation oncologist prepared the dog’s treatment plan for the following week, she saw on the
CT scan that the tumor was also invading the colon. That changed the equation, with the risks from radiation to that area outweighing the benefits of treating with radiation. We then changed our recommendation: No Cyberknife for Chandler.
Since the cancer was more advanced than originally thought, we went to Plan B. That’s what I would do for Paige, I told Chandler’s owners. We started chemotherapy and pain medications, including a non-steroidal anti-inflammatory drug or NSAID, which can also have anti-cancer properties for his form of cancer. Chandler did well after his first chemotherapy treatment, even though his white blood cell count got a little low.
At that visit, they told me they were supposed to go out of the country for an important family event, a trip that had been planned many months ago. They had friends willing to make the three-hour trip to bring Chandler in for his next chemo. Should they cancel their trip, they asked? What would I do in their position? I told them that while I do not have a crystal ball, he would likely be fine having friends bring him in. He was stable and doing well.
None of us knew they would never seem him again.
Plan B fails, and Plan C looms
The friends brought Chandler in for his second chemotherapy treatment as planned. They also adored the little dog and were happy to make the long trip to help. When they arrived, they told me Chandler had been vomiting. I knew it was unlikely the first chemotherapy treatment was responsible, based on the timing. Vomiting from chemotherapy typically occurs within a week of treatment, and it had been two weeks. Some cancers can cause vomiting, but Chandler’s wasn’t typically one of them. It had to be something else.
Blood work quickly determined that Chandler was in severe kidney failure, which definitely causes nausea and vomiting. On the ultrasound, we could see the tumor was even more advanced. The urine flow was being blocked by the tumor, and that was causing the kidney failure.
[tweetthis]Should a veterinarian treat a patient as if the pet were her own?[/tweetthis]
I called his owners, and filled them in as we went over the options. We even discussed stopping treatment, before they opted for Plan C. Chandler entered our ICU for aggressive fluid therapy, and we scheduled a surgery for the next day to open up both ureters with stents. Stenting is a sort of propping-open procedure used to open up arteries, or in this case, ureters that have a blockage. The plan was to restart chemotherapy treatments after Chandler recovered from the surgery.
I kissed Chandler as he went into the operating room with my surgical colleague, knowing he was in the best possible hands. I was in appointment when I was called back to the OR, my heart sinking. The surgeon had found something we could not fix: The cancer had spread all over Chandler’s abdomen, a situation much more advanced than we could see on ultrasound.
Stents were not going to help Chandler. At this point, even our Plan C was not a fair option for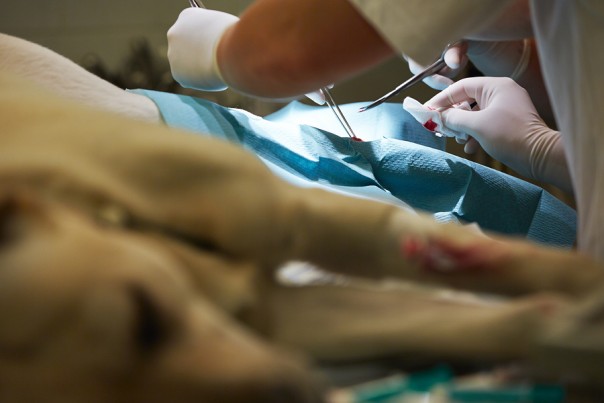 Chandler.
Chandler.
It was time for the kind of phone call all veterinarians hate to make. I called the family and told them we should euthanize while Chandler was still under anesthesia. I didn’t believe it was it fair to wake him up after what we had seen. The family was still out of the country, and they couldn’t get home for days. Yes, I told them, this is what I would do for Paige. So they consented, far away, and unable to say their goodbyes.
Sobs and self-examination
I hung up the phone and sobbed. As promised, I went into the OR and kissed Chandler goodbye, as if he were my own. And then it was time for self-examination.
As an oncologist I work with the best internist, surgeon, technicians, and support staff. We have advanced treatment options like CyberKnife radiation and ureteral stents. All the money, the best health care, and it still didn’t matter. Sometimes, even as a cancer specialist it still shocks me how quickly and aggressively cancer can progress.
[tweetthis]Sometimes, even as a cancer specialist, it shocks me how quickly cancer can progress.[/tweetthis]
I could not help Chandler, and that hard truth is defeating, humbling, and depressing. I mourn for the family and thank them for the trust. I am sorry we could not do more. All I could do was end his suffering.
This is a large part of why I am always hesitant when someone asks me to treat her pet as if the animal were my own. I would go pretty far for mine, especially Paige was still with me, perhaps further than most people would or could.
When is the time is right to stop treating? I struggle with it with my own pets. I was trained to help pets with cancer. I am an advocate for cancer treatment. Cancer is not a death sentence. Most pets that we treat tolerate treatment well, and live not only longer, but they live well – even during chemotherapy treatment. I know all this, but …
I also know that sometimes there are no more options. Whether deciding to treat or to euthanize, we all need support and we struggle to do what is best.
I had treated Chandler as if he were my own, and my heart broke because I did.
[tweetthis]I am an advocate for cancer treatment. Cancer is not a death sentence.[/tweetthis]
